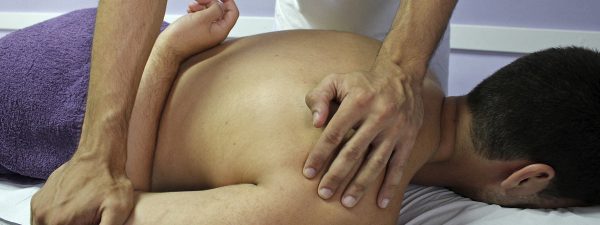
Expert Physiotherapy
Services & Care
Let's Work Together!
Specialized care for pain management, rehabilitation, sports injuries and more. Our expert team helps you regain movement and live pain-free.
About Our Physiotherapy Services & Care
"Our Expertise, Your Effort"
ProPhysiotherapy is an elite physiotherapy clinic dedicated to providing expert care with a personal touch. With over 25 years of experience, our team of highly skilled physiotherapists is committed to helping you achieve optimal health and wellbeing.
Whether you're recovering from an injury, managing chronic pain, or looking to improve your physical performance, we offer comprehensive services tailoured to your individual needs.
Expert Team
Our physiotherapists have extensive training and experience in a wide range of specialties.
Personalized Care
We develop customized treatment plans tailored to your specific needs and goals.
Convenient Hours
We offer flexible appointment times to accommodate your busy schedule.
Evidence-Based
Our treatments are based on the latest research and proven clinical methods.
Comprehensive Physiotherapy Care & Services
We offer a comprehensive range of physiotherapy services to help you recover, manage pain, and improve your quality of life.
Meet Our Expert Team
Our team of highly skilled physiotherapists is dedicated to providing exceptional care tailored to your individual needs.
Specialized Care
Discover our specialized services designed to meet your unique health and wellness needs.

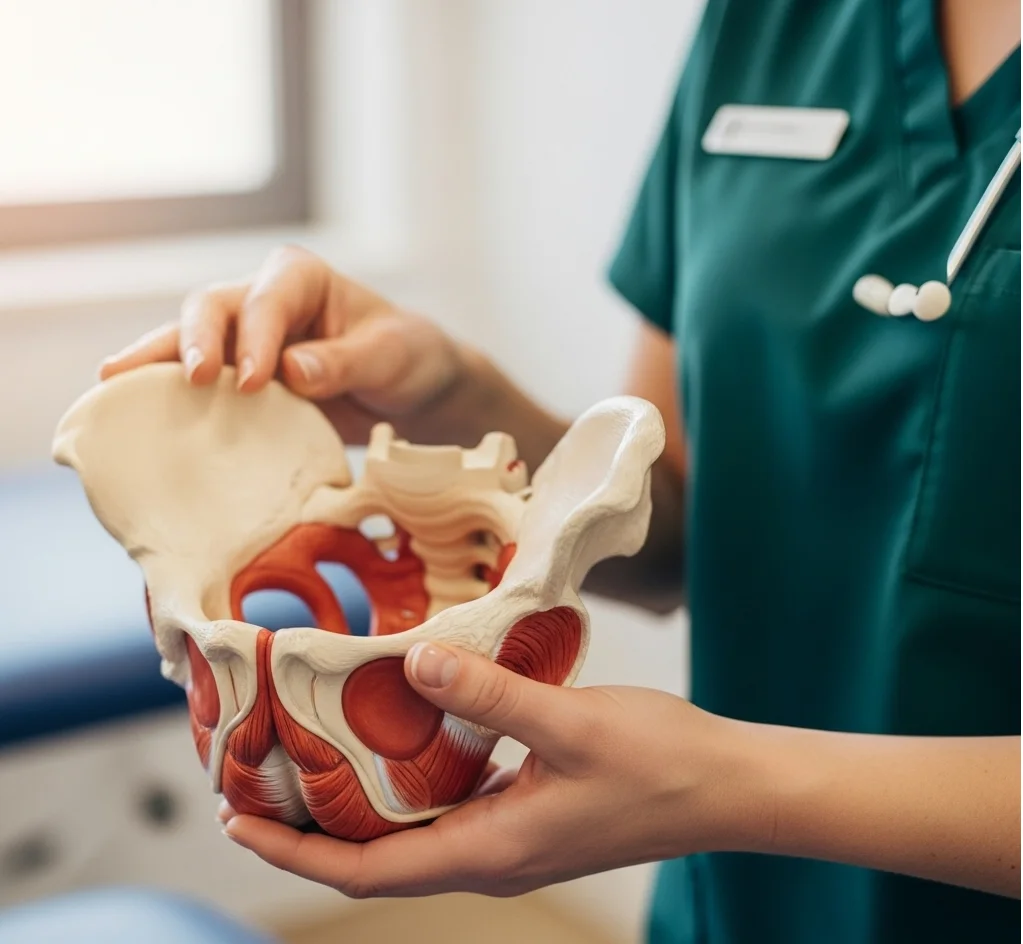
Women's Health
Expert care for pregnancy, postnatal recovery, and pelvic health.

Clinical Pilates
Therapeutic Pilates instruction for rehabilitation and wellness.
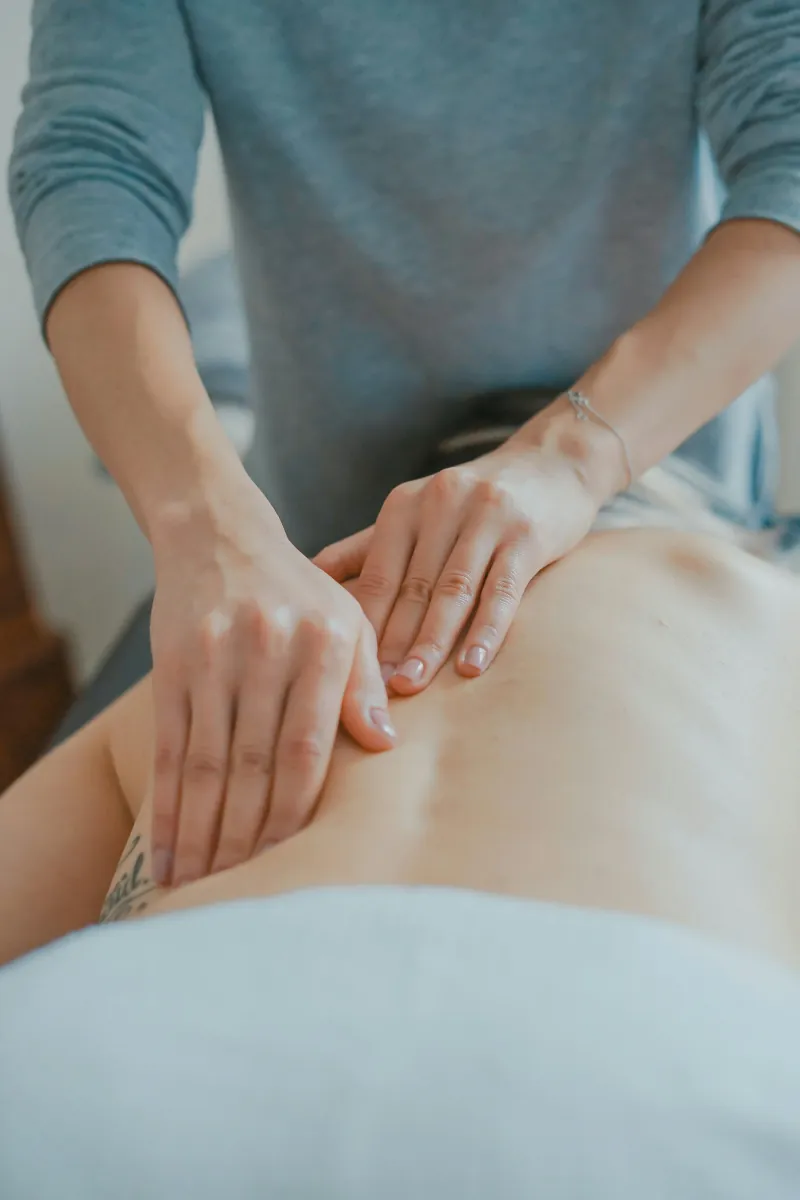
Massage Therapy
Professional therapeutic massage for recovery and performance.

Pricing
Transparent pricing for all our services and treatments.
Conditions We Treat
Our experienced physiotherapists specialize in treating a wide range of musculoskeletal conditions. Find expert care tailored to your specific needs.
Back Pain
Comprehensive treatment for acute and chronic back pain
See How We HelpFrozen Shoulder
Specialist care for adhesive capsulitis and shoulder stiffness
See How We HelpACL Tear or Injury
Expert rehabilitation for anterior cruciate ligament injuries
See How We HelpPlantar Fasciitis
Effective treatment for heel and foot pain
See How We HelpTennis Elbow
Relief from lateral epicondylitis and elbow pain
See How We HelpNeck Pain
Treatment for cervical pain and stiffness
See How We HelpAchilles Tendinopathy
Specialized care for achilles tendon injuries
See How We HelpCarpal Tunnel Syndrome
Non-surgical treatment for wrist and hand pain
See How We HelpWhat Our Patients Say
Testimonials from our satisfied patients who have experienced our expert physiotherapy care.
Latest from Our Blog
NEWExpert insights, health tips, and the latest in physiotherapy and wellness
Popular Health Topics to Learn About
Explore our most read articles covering injuries, treatments, and wellness tips
Insurance Partners
We work with all major health insurance providers to ensure you get the care you need.
BUPA
One of the UK's leading healthcare providers
AXA PPP Healthcare
Global leader in insurance and healthcare
Vitality Health
Innovative health and life insurance
Aviva
UK's largest insurance provider
WPA
Not-for-profit health insurance provider
Cigna
Global health service company
Simply Health
Healthcare solutions provider
Allianz
Worldwide insurance and financial services
Please contact your insurance provider before booking to confirm coverage details.
Ready to Begin Your Journey to Recovery?
Take the first step towards improved health and wellness. Book your consultation with one of our expert physiotherapists today.
Get In Touch
Have a question or want to learn more about our services? Send us a message and we'll get back to you within 24 hours.
Prefer to contact us directly? 020 8879 1555 or enquiries@prophysiotherapy.co.uk


.webp)
.webp)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)


.jpg)